Definition and Incidence
Male urinary incontinence is an oftentimes overlooked and underdiagnosed problem.
Recent reports have shown that as many as 9-13% of American men suffer from urinary incontinence.
Urinary incontinence is not a disease or a normal consequence of aging, therefore, most cases can be cured or improved. It is a symptom with many causes and is the medical term used to describe the condition of not being able to control the flow of urine from your body. It usually happens because the bladder sphincter is damaged or scarred and cannot squeeze or close off the urethra. This means urine can leak or flow freely from the bladder.
Physiology
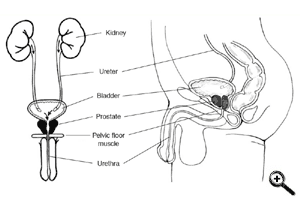
Male continence is maintained by two sphincters: internal and external. The internal sphincter is part of the bladder neck and is under involuntary or reflex control by higher centers of urination in the brain. The external sphincter, which is part of the pelvic floor
muscles, is a voluntary sphincter and is actively relaxed at the time of urination. Oftentimes, the internal sphincter is removed or damaged as is the case during radical prostatectomy or bladder neck surgery such as TURP. In these situations the man must rely entirely on the external sphincter to maintain continence. Unfortunately, the external sphincter may be damaged as well during these same types of surgeries rendering the patient incontinent.
Classification and Causes of Male Incontinence
Male urinary incontinence can be classified into 4 different categories:
- Stress Incontinence – Occurs when you leak urine during physical activity such as exercise, walking, lifting, coughing and sneezing.
- Urge Incontinence – Occurs when you have an overwhelming need to urinate and are not able to hold urine long enough to reach the toilet.
- Mixed Incontinence – A combination of stress and urge incontinence, where you have symptoms of both conditions.
- Overflow Incontinence – When your bladder never completely empties which causes urine to leak. This type of incontinence is found in men with prostate enlargement, scars/strictures of the urethra or bladder neck and can also be due to dysfunctional bladder function, as seen in
diabetic patients.
Diagnosis of Male Urinary Incontinence
Diagnosis of the specific type of incontinence in men can be more complex than in women. The typical evaluation includes a detailed medical history and physical examination. Sometimes your physician will request a voiding diary or pad weight log to determine the nature and degree of incontinence. It is important to rule out simple causes of male urinary incontinence such as urinary tract infection with a formal urine culture, non-invasive flow rate and residual urine measurement. Additional testing should include complex urodynamics and cystoscopy. |
|
Treatment Options for Male Urinary Incontinence
Behavioral Techniques – Scheduled toileting is one technique that puts a man on a regular voiding regimen, and is typically recommended for the frail and elderly. Bladder retraining is a way men can go to the bathroom at specific times in the day where times can gradually be extended to longer intervals. This type of therapy is effective is treating urge and mixed incontinence.
Pharmacological Depending on symptoms, medications can be given to help men with incontinence. Anticholinergic agents can be used as first-line treatments for urge incontinence because they inhibit detrusor contraction, and may help increase bladder capacity. Stress incontinence is typically treated with surgery.
Biofeedback/Electrical Stimulation Biofeedback/Electrical Stimulation is practiced to help people gain awareness and control of their urinary tract muscles. The principle of biofeedback is simple: a variety of instruments are used to record small electrical signals that are given off when specific muscles are squeezed to urinate. These muscle squeezings are then converted into audio (hearing) and/or visual (seeing) signs that patients can recognize and learn in order to control muscular activity. With biofeedback, weak muscles can be better activated on demand, overly tense muscles can be relaxed and overall muscle activity can be coordinated.
Surgical Options Surgical procedures are available to treat male urinary stress incontinence.
- Injections of bulk-producing agents, such as collagen, into the urinary sphincter.
- Implanting a “male sling,” a device designed to support the muscles around the urethra. The AMS AdVance Male Sling System is highly effective, minimally invasive procedure to correct mild to moderate stress urinary incontinence.
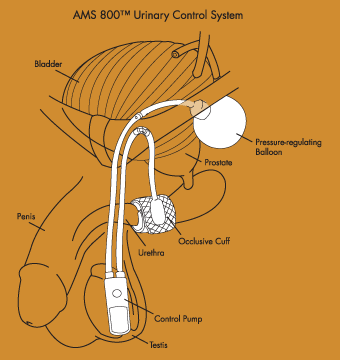
- Implanting an artificial urinary sphincter, which mimics the function of a normal, healthy urinary sphincter. Currently the only artificial urinary sphincter available, the AMS 800
Urinary Control System is an effective solution for moderate to severe stress urinary incontinence following prostate surgery.
|